Plantar warts are warts that are only found on the feet, hence the term “plantar”, which means “relating to the foot.” They are caused by the human papillomavirus, or HPV, and occur when this virus gets into open wounds on the feet. The warts themselves are hard bumps on the foot. They are easily recognizable, mostly found on the heels or ball of the foot. Plantar warts are non-malignant, but they can cause some pain, discomfort, and are often unsightly. Removing them is a common step toward treating them.
Plantar warts can cause some pain while standing, sometimes felt as tenderness on the sole of your foot. Unless the wart has grown into the foot behind a callus, you will be able to see the fleshy wart. A podiatrist should only be consulted if there is an excessive amount of pain. Plantar warts are not cancerous or dangerous, but they can affect your walking and continually reappear. Anyone who suffers from diabetes or a compromised immune system disease should seek out care immediately.
Podiatrists are easily able to diagnose plantar warts. They usually scrape off a tiny bit of the rough skin to make tiny blood clots visible and examine the inside of warts. However, a biopsy can be done if the doctor is not able to diagnose them from simply looking at them. Although plantar warts usually do not require an excessive amount of treatment, there are ways to go about removing them. A common method is to freeze them off using liquid nitrogen, removing them using an electrical tool, or burning them off via laser treatment. For a less invasive treatment option, topical creams can be used through a doctor’s prescription. This treatment method takes more time, however. Keep the wart covered for protection in between daily treatments.
The best way to avoid developing plantar warts is to avoid walking barefoot in public places. Avoid this especially if you have open sores or cuts on your feet. It is also important to avoid direct contact with warts in general, as they are highly contagious.
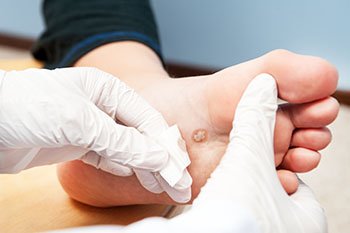
When the outer layer of skin on the sole of the feet comes in contact with the human papilloma virus, thickened growths called plantar warts can develop. The virus—which can lurk in public showers, pools, and locker rooms—enters through tiny breaks in the skin on the bottom of feet. These flat, rough masses sometimes have tiny black “dots” in the center, which are actually tiny blood vessels. They can be uncomfortable at times—especially if they occur on weight-bearing areas of the feet and toes. While verrucas can often heal on their own, they can be stubborn, and you may want to see a podiatrist to help get rid of them.
Plantar warts can be very uncomfortable. If you need your feet checked, contact Dr. Alexander Terris from Total Foot Care. Our doctor will assist you with all of your foot and ankle needs.
About Plantar Warts
Plantar warts are the result of HPV, or human papillomavirus, getting into open wounds on the feet. They are mostly found on the heels or balls of the feet.
While plantar warts are generally harmless, those experiencing excessive pain or those suffering from diabetes or a compromised immune system require immediate medical care. Plantar warts are easily diagnosed, usually through scraping off a bit of rough skin or by getting a biopsy.
Symptoms
Treatment
To help prevent developing plantar warts, avoid walking barefoot over abrasive surfaces that can cause cuts or wounds for HPV to get into. Avoiding direct contact with other warts, as well as not picking or rubbing existing warts, can help prevent the further spread of plantar warts. However, if you think you have developed plantar warts, speak to your podiatrist. He or she can diagnose the warts on your feet and recommend the appropriate treatment options.
If you have any questions please feel free to contact our office located in Wilmington, DE . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Read more about All About Plantar Warts
Do you suffer from heel pain when you get up in the morning? If so, you should seek the professional help of your podiatrist and have a proper diagnosis performed. Heel pain can be caused by several different foot-related conditions.
Ankle foot orthotics are shoe inserts that offer support to control the placement and movement of the ankle, correct deformities, and compensate for weakness. These inserts are used to stabilize the foot and ankle and provide toe clearance during the swing phase of gate.
Athletes often suffer foot problems because their feet are not being supported within the shoe. Ankle and foot orthotics are custom made inserts that alleviate stress on the foot. However custom orthotics should be prescribed by a podiatrist who specializes in customized footwear and orthotics design. These inserts are used by athletes for different reasons. Runners use orthotics to absorb shock at heel contact and to set up the forefoot for push-off. Basketball players wear them to control their forefeet while jumping and running.
The two main types of orthotics are over-the-counter orthotics and custom-made orthotics. To be eligible for custom orthotics, an examination of the foot and ankle will need to be completed. Afterward, both the foot and ankle will need to be casted and fitted for the proper orthotic. When the fitting process is complete, adjustments can be made to make sure everything fits perfectly.
Over the counter orthotics tend to be more popular than custom fit ones. Athletes who have less severe aches and pains in the foot, ankle or lower back area can use the over-the-counter version of orthotics. Unfortunately, over-the-counter orthotics tend to not work in treating severe injuries or ailments. Whenever you suspect you may need an ankle foot orthotic, you should consult with your podiatrist to determine which type of orthotic is right for you.
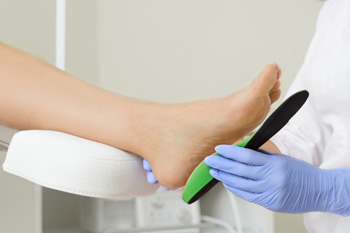 Orthotics are shoe inserts that are designed to correct a variety of foot-related problems including foot pain, knee pain, and lower back pain as well. Common ways that orthotics may address these issues include aligning the feet, relieving pressure on the feet, helping the foot function, supporting the ankle, or reducing the chance for injuries. Orthotics are also often used for patients with plantar fasciitis, arthritis, bunions, flat feet, heel spurs, high arches, and hammertoe. Orthotics can be customized, and a podiatrist can use a variety of methods such as a physical exam, imaging (X-rays, bone scans, MRIs), and observations of your walking pattern to determine the right customizations that are needed for you. Patients who are interested in orthotics should consult with a podiatrist.
Orthotics are shoe inserts that are designed to correct a variety of foot-related problems including foot pain, knee pain, and lower back pain as well. Common ways that orthotics may address these issues include aligning the feet, relieving pressure on the feet, helping the foot function, supporting the ankle, or reducing the chance for injuries. Orthotics are also often used for patients with plantar fasciitis, arthritis, bunions, flat feet, heel spurs, high arches, and hammertoe. Orthotics can be customized, and a podiatrist can use a variety of methods such as a physical exam, imaging (X-rays, bone scans, MRIs), and observations of your walking pattern to determine the right customizations that are needed for you. Patients who are interested in orthotics should consult with a podiatrist.
If you are having discomfort in your feet and would like to try orthotics, contact Dr. Alexander Terris from Total Foot Care. Our doctor can provide the care you need to keep you pain-free and on your feet.
What Are Orthotics?
Orthotics are inserts you can place into your shoes to help with a variety of foot problems such as flat feet or foot pain. Orthotics provide relief and comfort for minor foot and heel pain but can’t correct serious biomechanical problems in your feet.
Over-the-Counter Inserts
Orthotics come in a wide variety of over-the-counter inserts that are used to treat foot pain, heel pain, and minor problems. For example, arch supports can be inserted into your shoes to help correct overarched or flat feet, while gel insoles are often used because they provide comfort and relief from foot and heel pain by alleviating pressure.
Prescription Orthotics
If over-the-counter inserts don’t work for you or if you have a more severe foot concern, it is possible to have your podiatrist prescribe custom orthotics. These high-quality inserts are designed to treat problems such as abnormal motion, plantar fasciitis, and severe forms of heel pain. They can even be used to help patients suffering from diabetes by treating foot ulcers and painful calluses and are usually molded to your feet individually, which allows them to provide full support and comfort.
If you are experiencing minor to severe foot or heel pain, it’s recommended to speak with your podiatrist about the possibilities of using orthotics. A podiatrist can determine which type of orthotic is right for you and allow you to take the first steps towards being pain-free.
If you have any questions please contact our office located in Wilmington, DE . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Read more about Ankle Foot Orthotics for AthletesHave you ever gotten up from a chair or out of bed in the morning, and upon taking that first step, feel like your heel has stepped on a tack? Many people experience a feeling of sharp pain which radiates into their arch from their heel and which does not allow them to put their heel on the floor. Sometimes they need to sit back down, stand only on their toes and use the wall for balance. If you can take a few steps, it seems to go away and lessen, allowing you to then resume your activity. Later, throughout your day and after a period of rest, it can happen again. If this sounds familiar you may be suffering from your first attack of heel pain.
Heel pain is a debilitating condition that affects day to day activities. Running and walking both causes stress on the heel because the heel is the part of the foot that hits the ground first. This means that the heel is taking on your entire weight. Diagnosis and treatments for heel pain can be easily found through your podiatrist.
Plantar Fasciitis
One of the main causes of heel pain is a condition known as plantar fasciitis. The plantar fascia is a band of tissue that extends along the bottom of the foot, from the toe to the bottom of the heel. A rip or tear in this ligament can cause inflammation of these tissues, resulting in heel pain. People who do not wear proper fitting shoes are often at risk of developing problems such as plantar fasciitis. Unnecessary stress from ill-fitting shoes, weight change, excessive running, and wearing non-supportive shoes on hard surfaces are all causes of plantar fasciitis.
Achilles Tendonitis
Achilles tendonitis is another cause of heel pain. Similar to plantar fasciitis, inflammation of the Achilles tendon will cause heel pain due to stress fractures and muscle tearing. A lack of flexibility of the ankle and heel is an indicator of Achilles tendonitis. If left untreated, this condition can lead to plantar fasciitis and cause even more pain on your heel.
Heel Spur
A third cause of heel pain is a heel spur. A heel spur occurs when the tissues of the plantar fascia undergo a great deal of stress, leading to a separation of the ligament from the heel bone entirely. This results in a pointed fragment of bone on the ball of the foot, known as a heel spur.
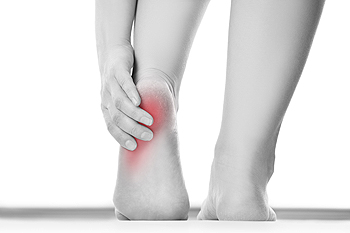
Heel pain is a common ailment which may be caused by an irritation of the nerves, arthritis, tendonitis, stress fractures in the heel, a cyst, or—most commonly—plantar fasciitis. Plantar fasciitis occurs when the plantar fascia—the long band of connective tissue on the sole which links the heel bone to the toes—becomes torn, stressed, or otherwise damaged. Repetitive movements during sporting activities, having flat feet or high arches, obesity, prolonged standing, non-supportive footwear and other factors can all put undue stress on the plantar fascia and cause this painful condition to manifest. If you have heel pain of any kind, make an appointment with a podiatrist who can pinpoint the cause of your heel pain and treat it accordingly.
Many people suffer from bouts of heel pain. For more information, contact Dr. Alexander Terris of Total Foot Care. Our doctor can provide the care you need to keep you pain-free and on your feet.
Causes of Heel Pain
Heel pain is often associated with plantar fasciitis. The plantar fascia is a band of tissues that extends along the bottom of the foot. A rip or tear in this ligament can cause inflammation of the tissue.
Achilles tendonitis is another cause of heel pain. Inflammation of the Achilles tendon will cause pain from fractures and muscle tearing. Lack of flexibility is also another symptom.
Heel spurs are another cause of pain. When the tissues of the plantar fascia undergo a great deal of stress, it can lead to ligament separation from the heel bone, causing heel spurs.
Why Might Heel Pain Occur?
Treatments
Heel pain should be treated as soon as possible for immediate results. Keeping your feet in a stress-free environment will help. If you suffer from Achilles tendonitis or plantar fasciitis, applying ice will reduce the swelling. Stretching before an exercise like running will help the muscles. Using all these tips will help make heel pain a condition of the past.
If you have any questions please contact our office located in Wilmington, DE . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Read more about Heel PainBunions are large bony bumps at the base of the big toe. Medically known as hallux valgus, a bunion is a misalignment of the metatarsophalangeal joint, or big toe joint. The misalignment will generally worsen with time if left untreated.
The exact cause of bunions is unknown, with genetics seen as a potential cause. High heels and poorly-fitted footwear, rheumatoid arthritis, and heredity all seem to be potential factors behind the exacerbation of bunions. Women have been found to be more likely to develop bunions in comparison to men.
Bunions do not always produce symptoms. The best way to tell is if the big toe is pushing up against the next toe and there is a large protrusion at the base of the big toe. You may or may not feel pain. Redness, swelling, and restricted movement of the big toe may be present as well.
Podiatrists use a variety of methods to diagnose bunions. If there are symptoms present, podiatrists will first consider that it is a bunion. If not, a physical examination will be conducted to check function of the big toe. Finally, an X-ray may be taken to view the extent of the bunion and confirm it is a bunion.
Typically, nonsurgical methods are used to treat bunions, unless the bunion has become too misaligned. Orthotics, icing and resting the foot, roomier and better fitted shoes, taping the foot, and pain medication are usually utilized first. If the bunion doesn’t go away or causes extreme pain, surgery may be required. Surgeons will either remove part of the swollen tissue or bone to straighten the toe out.
If you have a bunion, it is recommended to see a podiatrist. The longer it is left untreated, the worse it may get. Podiatrists can properly diagnose and treat a bunion before it gets worse.
Custom orthotics, or shoe inserts, should be periodically replaced. Orthotics must fit properly to give you the best results. Protect your feet and ankles!
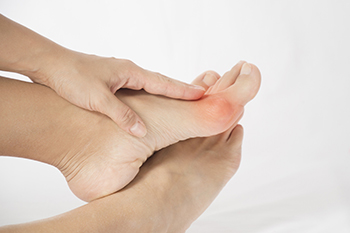 Bunions are bony growths that appear on the outer side of the foot at the base of the big toe joint. This is a deformity that may cause pain, swelling, redness, and difficulty wearing shoes and while walking. When left untreated, bunions tend to progressively worsen over time. As a bunion grows, it pushes the big toe towards the smaller toes, changing the shape of the foot in the process. The misaligned big toe may then push the second toe out of alignment. Bunions can also lead to arthritis in the big toe joints. Bunions can be managed and their progression can be slowed through a variety of conservative treatments, such as footwear modifications. Surgery may also be an option and can permanently correct a bunion. If you suffer from bunions, it is suggested that you see a podiatrist for treatment.
Bunions are bony growths that appear on the outer side of the foot at the base of the big toe joint. This is a deformity that may cause pain, swelling, redness, and difficulty wearing shoes and while walking. When left untreated, bunions tend to progressively worsen over time. As a bunion grows, it pushes the big toe towards the smaller toes, changing the shape of the foot in the process. The misaligned big toe may then push the second toe out of alignment. Bunions can also lead to arthritis in the big toe joints. Bunions can be managed and their progression can be slowed through a variety of conservative treatments, such as footwear modifications. Surgery may also be an option and can permanently correct a bunion. If you suffer from bunions, it is suggested that you see a podiatrist for treatment.
If you are suffering from bunion pain, contact Dr. Alexander Terris of Total Foot Care. Our doctor can provide the care you need to keep you pain-free and on your feet.
What Is a Bunion?
Bunions are painful bony bumps that usually develop on the inside of the foot at the joint of the big toe. As the deformity increases over time, it may become painful to walk and wear shoes. Women are more likely to exacerbate existing bunions since they often wear tight, narrow shoes that shift their toes together. Bunion pain can be relieved by wearing wider shoes with enough room for the toes.
Causes
Symptoms
In order to diagnose your bunion, your podiatrist may ask about your medical history, symptoms, and general health. Your doctor might also order an x-ray to take a closer look at your feet. Nonsurgical treatment options include orthotics, padding, icing, changes in footwear, and medication. If nonsurgical treatments don’t alleviate your bunion pain, surgery may be necessary.
If you have any questions, please feel free to contact our office located in Wilmington, DE . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Read more about What Are Bunions?